Abstract
Purpose: To explore the association of frailty with mortality, functional outcome, and health status after out-of-hospital cardiac arrest.
目的:探讨衰弱与院外心脏骤停后死亡率、功能结局及健康状况的关联。
Methods: This is a cohort-based secondary analysis of the Targeted Hypothermia versus Targeted Normothermia after out-of-hospital cardiac arrest (TTM2) trial, an international, prospective, multicentre study. Frailty was assessed using the Clinical Frailty Scale (1-9): fit (1-3), prefrail (4), frail (5), and severely frail (6-9). Main outcomes were mortality and poor functional outcome (modified Rankin Scale 4-6) at 6 and 24 months. Additional outcomes included neuroprognostication, withdrawal-of-life-sustaining-therapies (WLST), functional decline (retrospectively reported pre-arrest versus 6 month Glasgow Outcome Scale Extended score), health status (EQ-5D-5L, EQ-VAS), and life satisfaction at 6 and 24 months.
方法:本研究为基于队列的二次分析,数据来源于“院外心脏骤停后目标低温与目标常温对比试验(TTM2)”——一项国际、前瞻性、多中心研究。采用临床衰弱量表(CFS,评分1-9分)评估衰弱程度,分为:健康(1-3分)、衰弱前期(4分)、衰弱(5分)、重度衰弱(6-9分)。主要结局为6个月和24个月的死亡率及不良功能结局(改良Rankin量表评分4-6分)。次要结局包括神经预后评估、撤除生命支持治疗(WLST)、功能下降(回顾性报告的骤停前与6个月格拉斯哥结局量表扩展版[GOS-E]评分对比)、健康状况(EQ-5D-5L量表、EQ视觉模拟评分[EQ-VAS])及6个月和24个月的生活满意度。
Results: Of 1861 participants, 240 (13%) were prefrail, and 188 (10%) were frail or severely frail. Mortality and poor functional outcome increased significantly with greater frailty. Compared to fit participants, adjusted ORs (95% CI) for 6 month mortality were: prefrail 2.7 (1.8-3.8), frail 3.7 (1.9-7.1), and severely frail 8.9 (4.2-18.7); and poor functional outcome: prefrail 2.9 (1.9-4.2), frail 3.9 (1.9-8.1), and severely frail 35.4 (8.4-148.8). Severely frail participants underwent neuroprognostication less often (p < 0.001), while WLST was more common in the prefrail, frail and severely frail (p < 0.001). Prefrail and frail survivors tended to report more frequent functional decline and lower health status, though with individual variation.
结果:在1861例参与者中,240例(13%)为衰弱前期,188例(10%)为衰弱或重度衰弱。死亡率与不良功能结局随衰弱程度加重显著升高:与“健康”参与者相比,6个月死亡率的校正比值比(OR,95%置信区间)为:衰弱前期2.7(1.8-3.8)、衰弱3.7(1.9-7.1)、重度衰弱8.9(4.2-18.7);6个月不良功能结局的校正OR为:衰弱前期2.9(1.9-4.2)、衰弱3.9(1.9-8.1)、重度衰弱35.4(8.4-148.8)。此外,重度衰弱参与者接受神经预后评估的频率更低(p<0.001);而衰弱前期、衰弱及重度衰弱患者的撤除生命支持治疗(WLST)更常见(p<0.001)。衰弱前期与衰弱幸存者的功能下降更频繁、健康状况更差(尽管存在个体差异)。
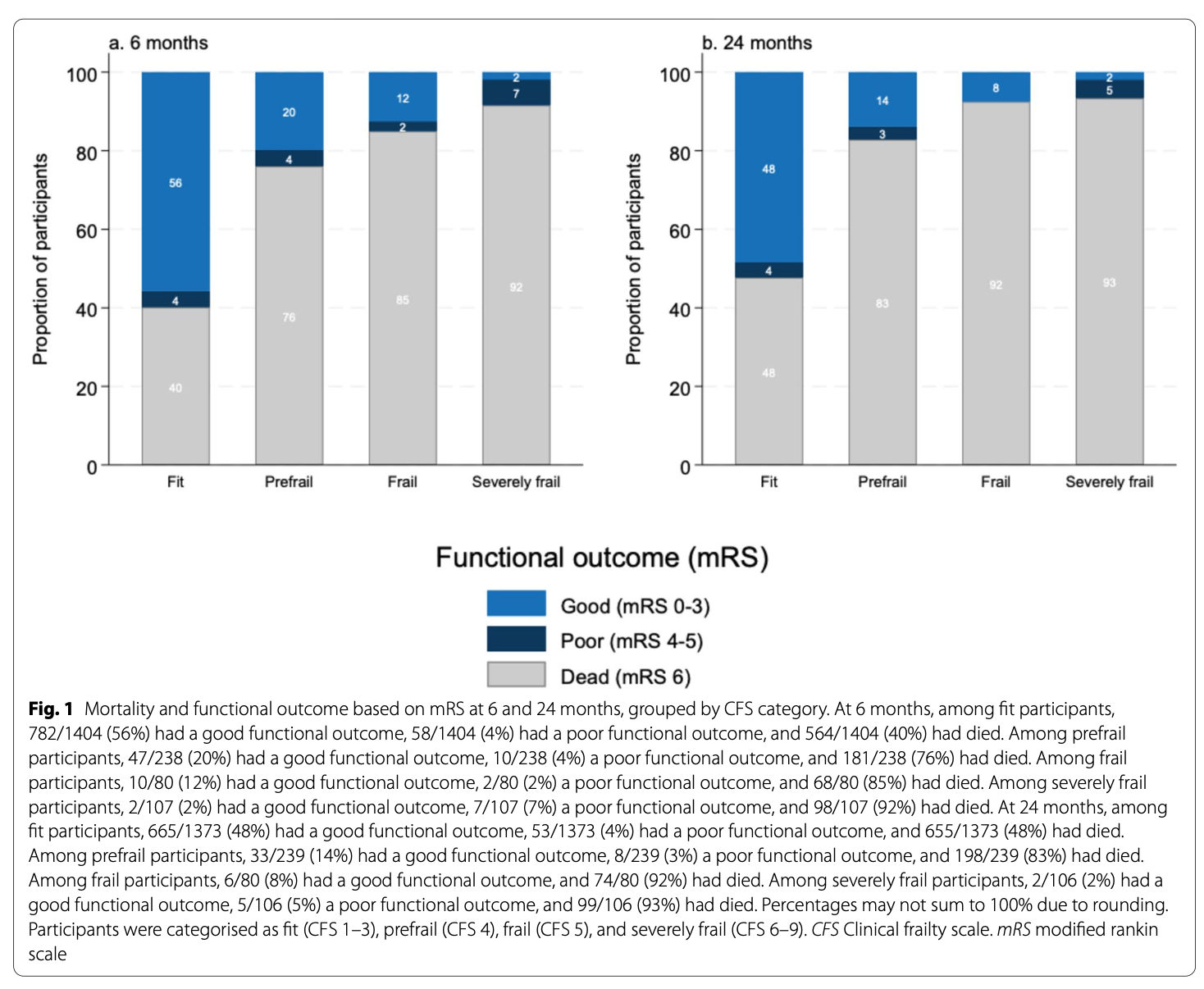
Conclusion: Frailty was associated with a significantly increased risk of mortality and poor functional outcome after out-of-hospital cardiac arrest. Findings suggest more frequent functional decline and lower overall health status in frail survivors.
结论:衰弱与院外心脏骤停后死亡率及不良功能结局风险显著增加相关。研究提示,衰弱幸存者更易出现功能下降,且整体健康状况更差。
原创文章(本站视频密码:66668888),作者:xujunzju,如若转载,请注明出处:https://zyicu.cn/?p=21248


 微信扫一扫
微信扫一扫  支付宝扫一扫
支付宝扫一扫 




