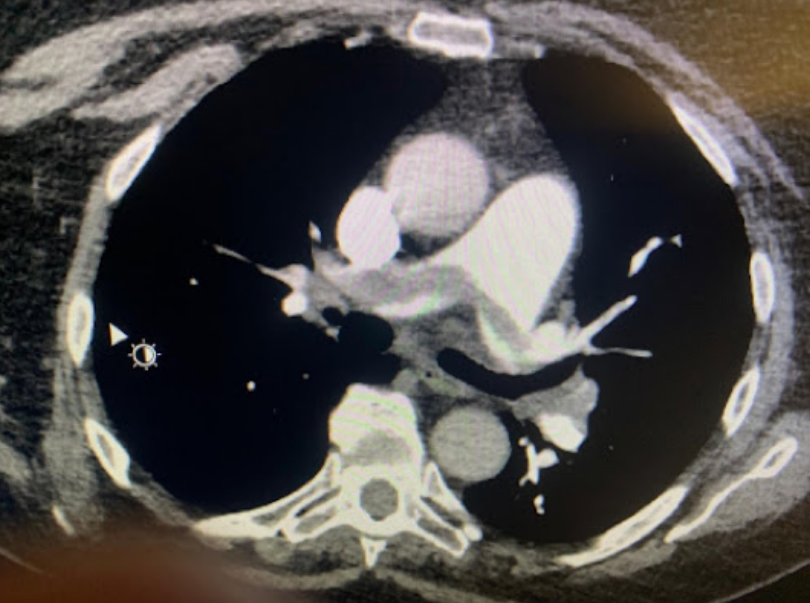
A 60-year-old female with a past medical history of obesity with associated obstructive sleep apnea, compliant with CPAP therapy, presents to the emergency department with worsening shortness of breath over the past three days. She states that she has also noted increased bilateral lower extremity edema. On examination, she has a temperature of 99 Farenheit, a blood pressure of 100/70 mmHG, a heart rate of 120 beats per minute, respiratory rate of 19 breaths per minute, and oxygen saturation is 91% on 5 litres of oxygen via nasal cannulae. She is placed on IV heparin, and a CT angiogram (CTA) chest, venous Doppler, and echocardiogram are ordered. The CTA reveals the findings seen here. Additionally a right ventricular/left ventricular (RV/LV) ratio of 1.3 is noted, with contrast reflux into the inferior vena cava.
What would be the most appropriate treatment strategy in this patient at this time?
A.Observe, escalate to non-rebreather mask, continue anticoagulation
B.Intubate, aggressive IV fluids with 0.9 NS, send for right heart catheterization
C.Escalate for catheter-based therapy
D.Intravenous alteplase 100 mg immediately
(PE)根据其肺栓塞评分指数归类为高风险(PESI评分约为130)。胸部CTA显示大的血栓负荷,在左右主肺动脉上可见鞍状PE。尽管她目前血流动力学稳定,但她存在失代偿风险,因此需要升级治疗。这将包括基于导管的溶栓治疗或基于导管的机械血栓切除术。基于多项试验的结果,由于慢性血栓性肺动脉高压(CTEPH)的并发症,残余肺阻塞导致结局较差。FLAIR和SEATTLE II试验证实,导管导向的溶栓剂和基于导管的机械血栓切除术均对次大面积PE患者有益。这两种治疗均显示RV/LV比值降低和右心室功能改善。该患者被送去接受机械血栓切除术,术后右心室血流动力学改善。
C
补充内容:

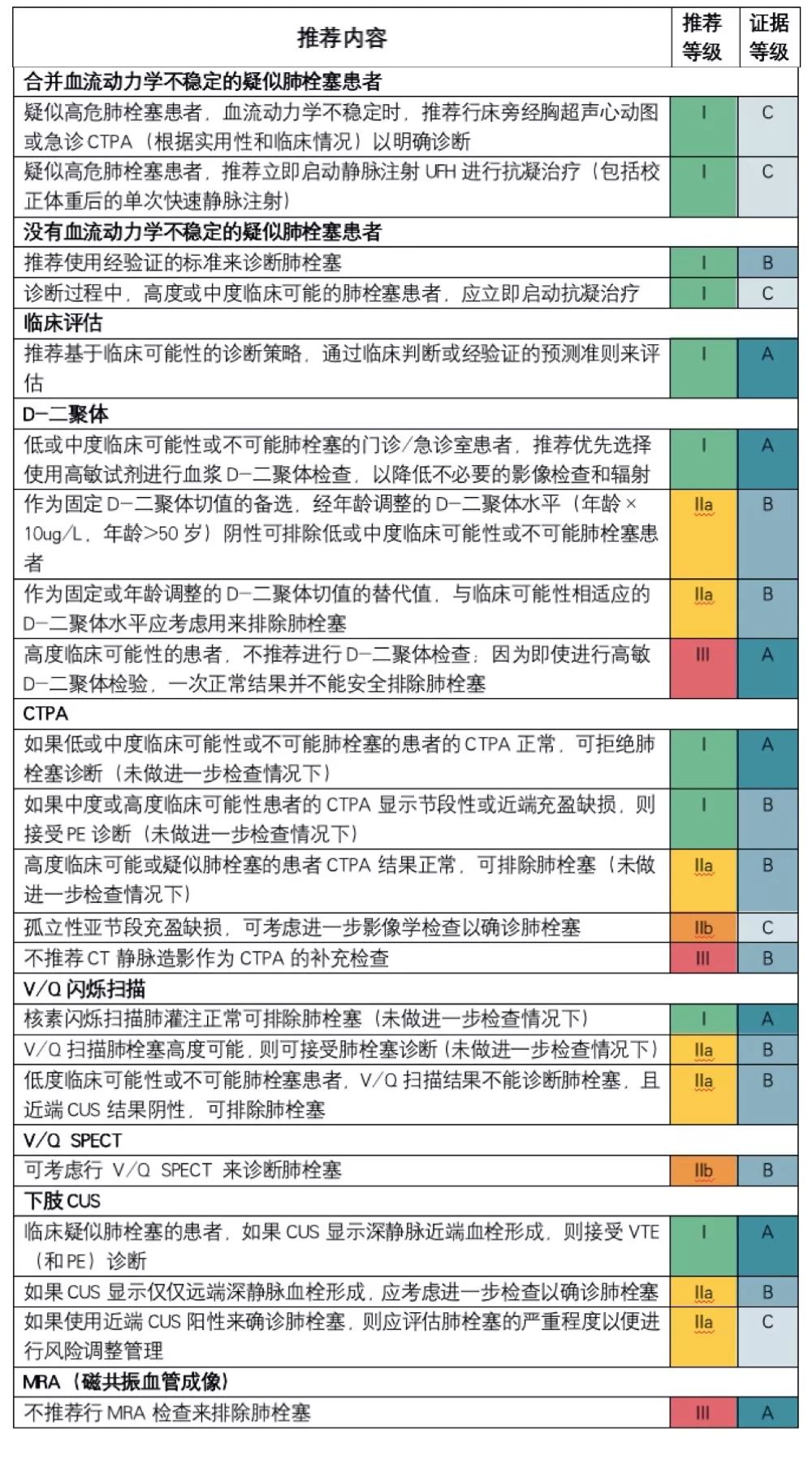
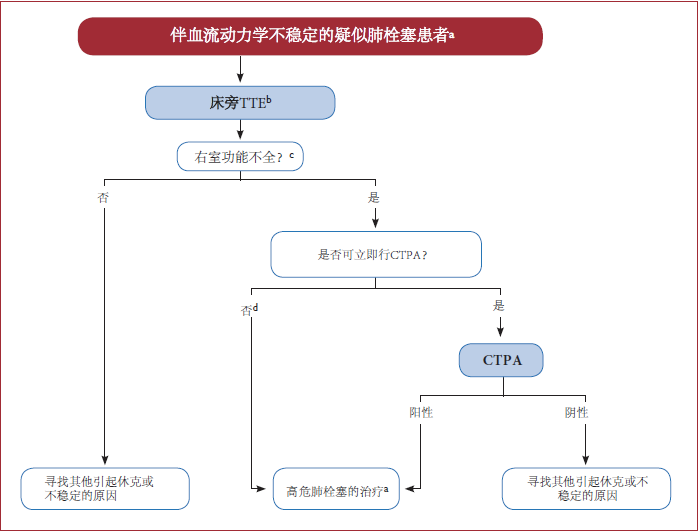
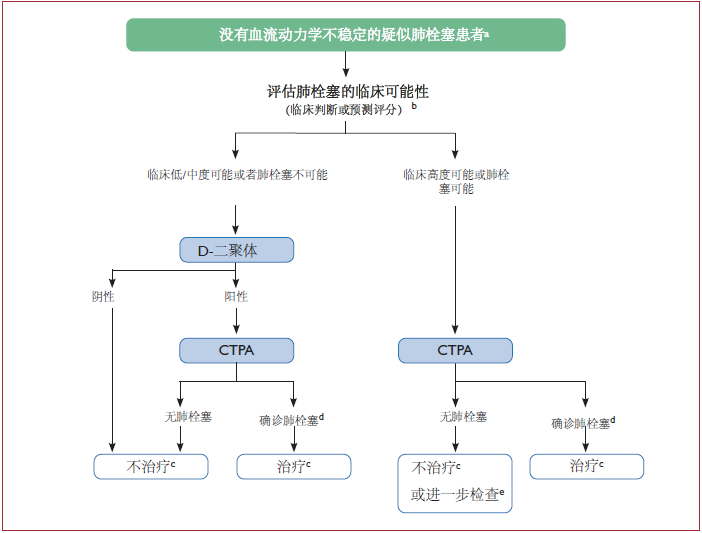
早期风险评估
肺栓塞的危险分层
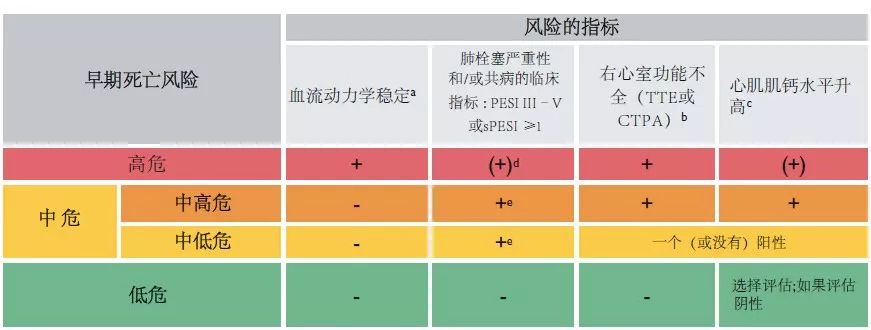
预后评估

急性期治疗
高危肺栓塞患者急性期治疗
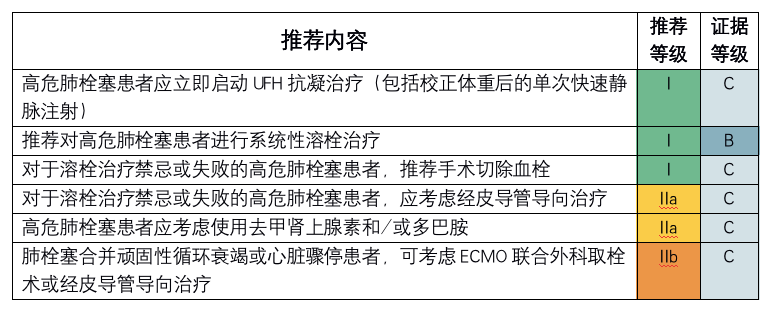
中危或低危肺栓塞患者急性期治疗
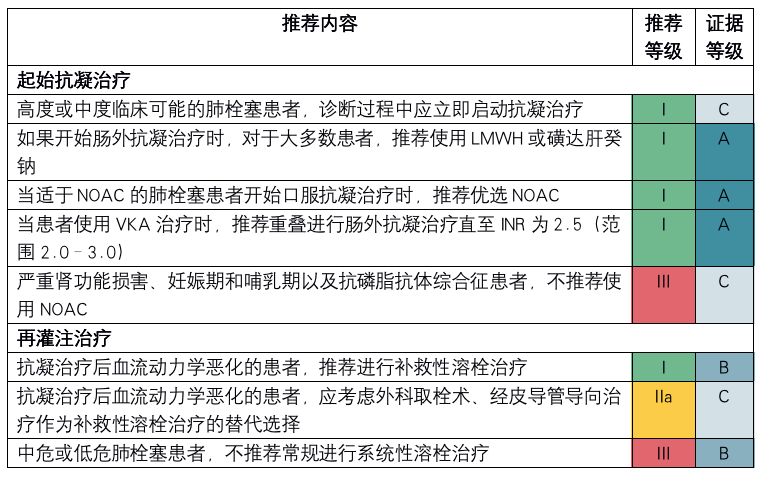
下腔静脉滤器

原创文章(本站视频密码:66668888),作者:xujunzju,如若转载,请注明出处:https://zyicu.cn/?p=8631

 微信扫一扫
微信扫一扫  支付宝扫一扫
支付宝扫一扫